The INTERCARE project ended in 2020.
Phase A: Model Development
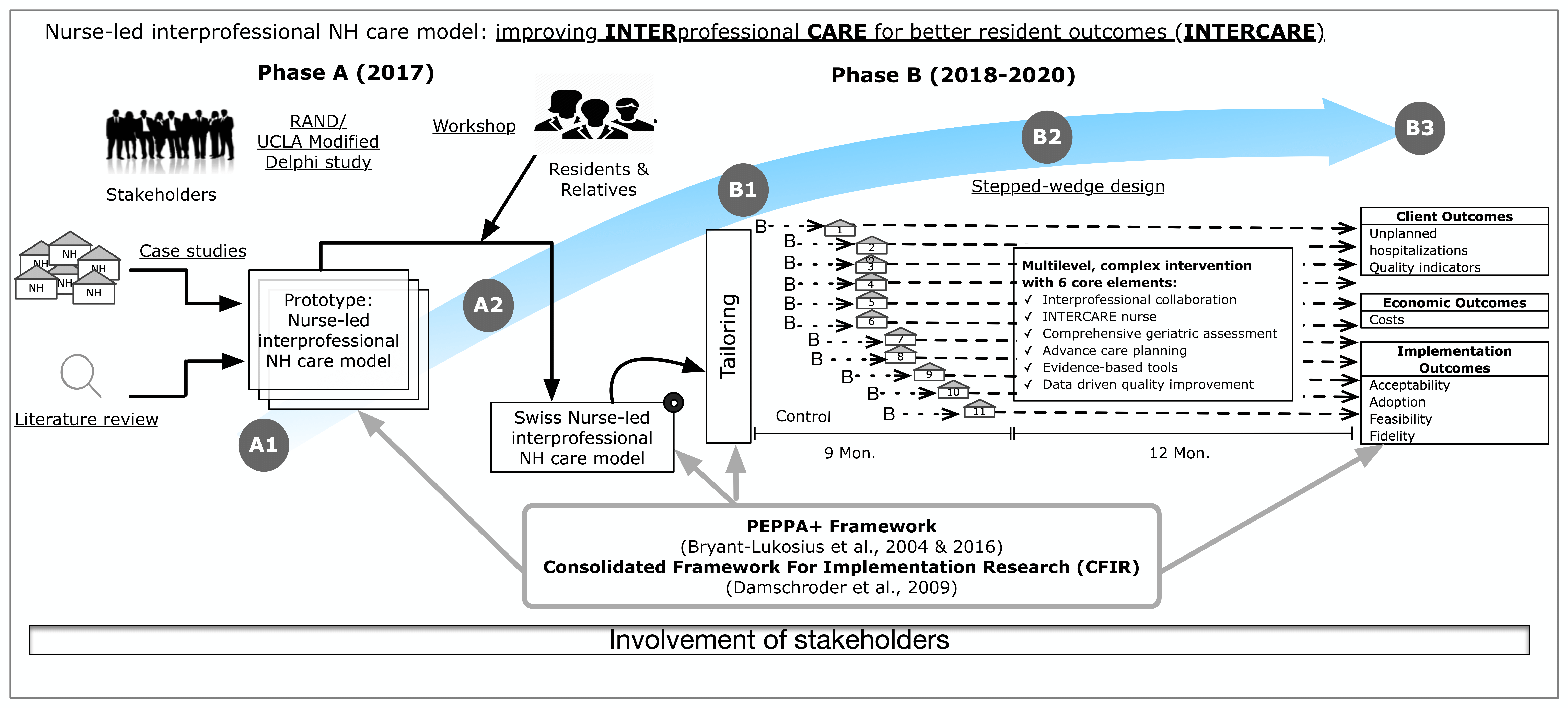
In phase A, a literature review and a descriptive analysis of national and international models of care already in place were carried out. With the participation of various stakeholders from residential LTC facilities, LTC facilities associations, professional associations, APN representations, education, policy, insurance companies and patient representatives in Switzerland, the nurse-led model of care (INTERCARE nurse-led model of care) focusing on the reduction of unplanned transfers was developed.
Phase B: Implementation and Evaluation
In Phase B, the newly developed interprofessional and nurse-led model of care was introduced and evaluated in 11 LTC facilities in the German-speaking Switzerland. Data was continuously collected during the study, which enabled a comprehensive analysis of the effects of INTERCARE on an array of outcomes.
Baseline Data Collection: the baseline data collection took place 3 months before the implementation phase, in all LTC facilities and included a survey of LTC facility’s characteristics and a staff survey. Starting at baseline, quality indicators and hospitalizations were measured and analyzed continuously. This allowed each LTC facility to serve first as a control and then as an intervention site.
Collection of evaluation data: the collection of evaluation data included both questionnaire surveys and interviews, as well as specifically collected outcome data and routine resident data, e.g. the RAI-MDS. The leadership of the LTC facilities, the care staff, physicians and the INTERCARE nurses were repeatedly questioned about the new nurse-led model of care and its impact.
Data was collected at various levels:
1. Clinical Outcomes. These include unplanned transfers, emergency department visits as well as quality indicators for the purpose of benchmarking. Data about staff satisfaction and recommendation as well as readiness for implementation and interprofessional collaboration during the implementation of the new nurse-led model of care were collected.
2. Implementation outcomes. Measurement of acceptability, feasibility, and fidelity to INTERCARE were measured throughout the implementation phase.
3. Costs. A cost-effectiveness analysis was conducted to measure the cost for the implementation of INTERCARE from the LTC facilities’ perspective and whether INTERCARE and how changes in hospitalization rates affected costs overall.